To diagnose BPH, doctors generally use the International Prostate Symptom Score questionnaire (IPSS) to evaluate the severity of symptoms. Designed by the American urological Association (AUA), the IPSS is an important tool to determine prostate problems at the early stage, to follow the progression of BPH and to track the treatment effects.
The IPSS consists of 7 questions, scored on a scale from 0-5:
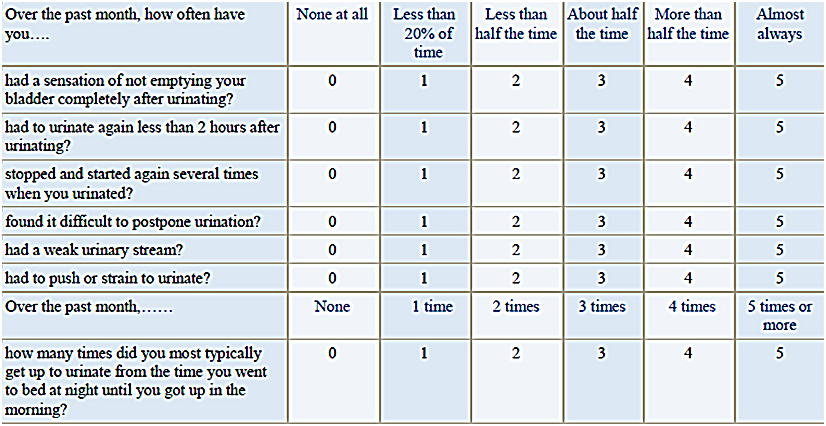
The symptoms are graded as:
mild: score 1 to 7
moderate: score 8 to 19
severe: score 20 to 35
Besides, doctors may also do some of the following tests to diagnose the condition:
Digital rectal examination (DRE)
The doctor inserts a gloved finger through the patient's anus into the rectum to assess the size, shape, symmetry and consistency of the prostate, to feel for nodules and hardness, and examine the rectum and anus at the same time. However, this test alone is not sufficient for diagnosing the degree of obstruction or the severity of the condition.
Urine test (urinalysis)
A urine test checks if there is blood in the urine, infection or proteinuria.
Prostate-specific antigen (PSA) blood test
PSA is a protein produced by the prostate. Elevated PSA levels may indicate prostate problems. PSA blood test can help screen for prostate cancer.
Uroflowmetry
Uroflowmetry measures the urine flow rate, the degree of obstruction and help to monitor treatment effects.
Transrectal ultrasound (TRUS)
An ultrasound test provides measurements of the prostate and reveals the amount of residual urine in the bladder.
Bladder function test
Straining to force out the urine due to difficult urination may cause weak bladder over time. Bladder function test is needed to check how well the bladder is working.
Urodynamics tests
Urodynamics tests measure the urine volume and pressure in the bladder, the urine flow rate and the residual urine in the bladder.
Cystoscopy
A lighted flexible telescope (cystoscope) is inserted into the urethra to examine the bladder for signs of obstruction or abnormalities.
In some cases, further tests may be needed to confirm the diagnosis. These tests include postvoid residual urine test, ultrasonography, intravenous urogram, magnetic resonance imaging (MRI), X-rays or intravenous pyelogram (IVP).